High blood pressure, also known as hypertension, is a condition of the body’s arteries. It occurs when the force of blood pumping through blood vessels remains consistently high over time. The increased force of the blood pushing against the walls of the vessels means the heart must work harder to pump the blood, increasing blood pressure. Uncontrolled high blood pressure can lead to serious health conditions, including stroke.
Track Your Blood Pressure Numbers
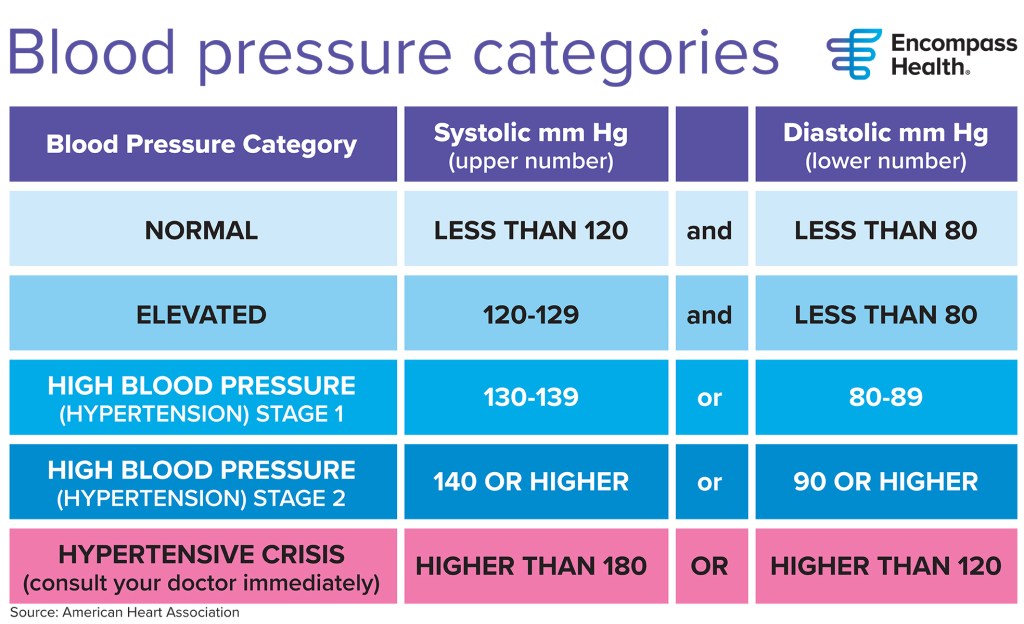
Understanding blood pressure readings and knowing your numbers is important. If your blood pressure is normal, it should be monitored at your annual healthcare check-up. If you have been diagnosed with hypertension, your doctor may recommend home blood pressure monitoring between medical visits. A high blood pressure diagnosis should always be confirmed by a healthcare professional—don’t try to manage it on your own.
High blood pressure is known as a silent killer because often there are no symptoms to alert you to the problem. When symptoms are present, they may not appear until your blood pressure has reached a serious level known as a hypertensive crisis. Signs of high blood pressure include:
- Headache
- Shortness of breath
- Nose bleeds
Treatment of High Blood Pressure
Controlling high blood pressure requires lifestyle changes and, in some cases, medication. If you have been told you have high blood pressure, your doctor will determine whether you need medication. If medication is recommended, you should take it exactly as prescribed. Other steps to lower blood pressure include:
- Stop smoking.
- Maintain a healthy weight.
- Avoid junk food and foods high in saturated or trans fats. Eat sugary treats and processed meats sparingly.
- Load your diet with healthy fruits and vegetables, whole grains, low-fat dairy products, poultry, nuts and fish.
- Focus on staying active. A healthy goal is 150 minutes of moderate intensity exercise weekly.
- Manage alcohol intake. Limit yourself to one drink per day if you are a woman or two drinks a day if you are a man.
- Ask your doctor what your blood pressure should be and try to maintain that reading.
High Blood Pressure and Stroke
Having high blood pressure increases the risk of different types of strokes:
- Ischemic stroke is caused by an obstruction in one of the large vessels that feeds blood to the brain. Eighty seven percent of all strokes are ischemic. In most cases, the obstruction is caused by a build-up of plaque in the vessel. The fatty plaque accumulates in the vessel restricting blood flow. A blood clot can also adhere to the plaque, creating a blockage. Brain cells can die rapidly when the blood source is cut off, so quick intervention is critical.
- A transient ischemic attack, also known as a mini stroke or TIA, occurs when a blood clot or plaque build-up causes a temporary blockage in blood flow to the brain. A TIA is typically brief, with symptoms lasting five minutes or less, and it resolves when the clot dissolves or the blockage is dislodged. TIAs are a serious warning sign for stroke. One-third of individuals who experience a TIA go on to have a stroke within a year.
- Hemorrhagic stroke happens when a blood vessel in the brain ruptures. Arteries damaged by high blood pressure can become weakened and are more likely to burst. Hemorrhagic strokes are less common than ischemic strokes but are also more deadly.
Hypertension is also linked to small vessel disease. The longer high blood pressure persists, the higher the risk of small vessel damage in the brain, leading to stroke or dementia.
Signs of Stroke
Sometimes symptoms of stroke are immediate and apparent, but other times they can be harder to recognize. Common stroke symptoms include:
- Facial drooping
- Changes in speech or inability to speak
- Arm or leg weakness or numbness
- Changes in vision, including double vision or vision loss
- Problems with balance or coordination
The American Heart Association and American Stroke Association developed an easy way to recognize the signs of stroke. The acronym F.A.S.T. was created to help people identify common symptoms of stroke and alert them to the need to call 9-1-1 immediately. F.A.S.T. stands for the following:
- Face drooping. Look for signs of facial weakness on one side. May be most noticeable when you ask the individual to smile.
- Arm weakness. Weakness or numbness in one arm is a sign of stroke. When both arms are raised, the weak arm will drift downward.
- Speech difficulty. Slurred speech or the inability to speak may be noted. It may also be difficult for the stroke victim to repeat simple sentences.
- Time to call 9-1-1. If you see the above signs – even if they only last a short time—get to the hospital immediately.
Stroke Rehabilitation
Learn more about stroke rehabilitation and the Encompass Health difference.
Learn MoreStroke Treatment
Every stroke is an emergency, and treatment depends on the type of stroke you had. The most effective stroke treatment must be administered within a few hours, so delays in diagnosing and treating stroke are associated with poorer outcomes. At the first sign of stroke, call for help and get to the hospital as soon as possible.
Ischemic stroke is often treated with a clot-busting medication called alteplase or r-TPA. The medication is given intravenously (IV) within four and a half hours of stroke symptom onset. Patients who are not eligible for r-TPA may undergo mechanical thrombectomy. This procedure is done by inserting a catheter with a wire-cage through an incision in the groin and threading it to the brain to retrieve the clot. It can only be used when the clot is lodged in a large artery.
Hemorrhagic stroke is treated through surgery or a less invasive endovascular procedure to stop the bleed.
How long it takes to recover after a stroke varies between individuals, but it’s generally believed that the most rapid recovery takes place in the first 90-120 days.
After a stroke, the right rehabilitation can make a substantial difference in recovery. In an inpatient rehabilitation hospital, a combination of physical, occupational and speech therapy help you recover from the effects of a stroke.
According to the 2016 adult stroke rehabilitation guidelines released by the American Heart Association, stroke patients should be treated at an inpatient rehabilitation facility, rather than a skilled nursing facility, whenever possible.
The content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.



