Pain is common after stroke, with an estimated 30 to 40% of stroke patients experiencing some form of pain, according to the American Stroke Association. If you or a loved one is recovering from stroke and experiencing pain, it’s important to first understand the underlying cause of your pain and speak with your healthcare team.
Patients who choose to recover in an inpatient rehabilitation hospital setting will work with therapists to address the causes of pain. Stroke patients are encouraged to continue coping techniques once they are at home.
Elizabeth Bartel, a physical therapist at Regional Rehabilitation Hospital in Phenix City, Alabama, said that while post-stroke pain can present challenges to recovery, there is reason to stay positive. “Know that with the right management—medically and physically—pain can get better,” she said.
What Causes Post-Stroke Pain
A stroke occurs when a blood vessel that carries oxygen and nutrients to the brain bursts or is blocked by a clot. When this happens, part of the brain cannot get the oxygen it needs and may be damaged. Stroke can cause nerve damage, muscle weakness and muscle stiffness—all of which can contribute to pain after stroke.
Types of Post-Stroke Pain
Shoulder pain
Shoulder weakness is a common condition after stroke. The shoulder joint can separate, creating a gap between the upper arm bone (humerus) and the shoulder joint itself. This is clinically known as shoulder subluxation. Common signs include decreased mobility, tingling and a sensation that the shoulder is out of alignment.
In other cases, the tissue that surrounds the shoulder thickens and creates scar tissue. As a result, shoulder movement may be limited and painful.
How it’s treated: Therapists focus on strengthening the shoulder girdle muscles to reconnect the humerus and the joint. This can be accomplished using range of motion exercises and proper instruction on how to position the affected shoulder.
If muscle activation in the shoulder is slow to return, your therapist might provide you with a sling to help with stability and reduce pain.

Central Post-Stroke Pain
CPSP is caused by damage to the central nervous system, which can lead to hypersensitivity. “An individual might jump at a light touch,” Bartel said. You might also experience changes in skin temperature, skin color and skin texture on the affected limb. CPSP is often described by stroke survivors as a burning sensation or aching and shooting pains.
How it’s treated: Therapists can help you overcome hypersensitivity with sensory retraining. These are simple exercises that re-introduce patients to new and different textures. For example, your therapist will gather objects with different textures and ask you to pick up the objects without looking at them to distinguish the difference among textures. Or your therapist will hand you various objects with your eyes open and give you time to sense how these objects feel. “We start with something soft and smooth such as a pillowcase or sheet and work up to rougher textures such as a washcloth or jeans,” Bartel said.
Pain related to hypersensitivity is also commonly treated with a transcutaneous electrical nerve stimulation (TENS) device. This battery operated unit can calm and soothe damaged nerves by delivering small electrical impulses through electrodes that have adhesive pads which are attached to the skin of the painful area. These devices are commonly used in hospitals, but can also be purchased for use at home.
Spasticity
Spasticity is a common post-stroke condition caused by an imbalance of signals from the central nervous system to the muscles. It occurs when a muscle involuntarily contracts when you move and usually affects the elbow, wrist and ankle. When a muscle can’t complete its full range of motion, the surrounding tendons and soft tissue can become tight, causing stiffness. This makes stretching the muscle much more difficult. In some cases, tightening of the muscles can become permanent. This is known as a contracture.
How it’s treated: Bartel said that gentle stretching exercises can help calm a spastic extremity. Therapists can also help you determine other factors that contribute to spasticity. “Often times if someone is frustrated while trying to complete a task, their spasticity can worsen. By identifying triggers, we can work through them together and find other solutions to prevent worsening the condition.”
Headaches
According to the American Stroke Association, headaches are often a confusing and misunderstood type of post-stroke pain. This is because the root of post-stroke headaches may be related to a number of causes. Most of the time, headaches are not a sign of a serious problem. However, as with any pain after a stroke, you should discuss it with your doctor to rule out any severe complications and explore treatment options.
How it’s treated: Your doctor will assess you to determine the potential cause of the headache. Treatment might include medication management and diet recommendations.
Coping with Post-Stroke Pain
Your doctor or therapists may recommend additional coping techniques to help manage pain after stroke. While techniques will vary from patient to patient, plans often include exercise programs, a well-balanced diet, stress management and support.
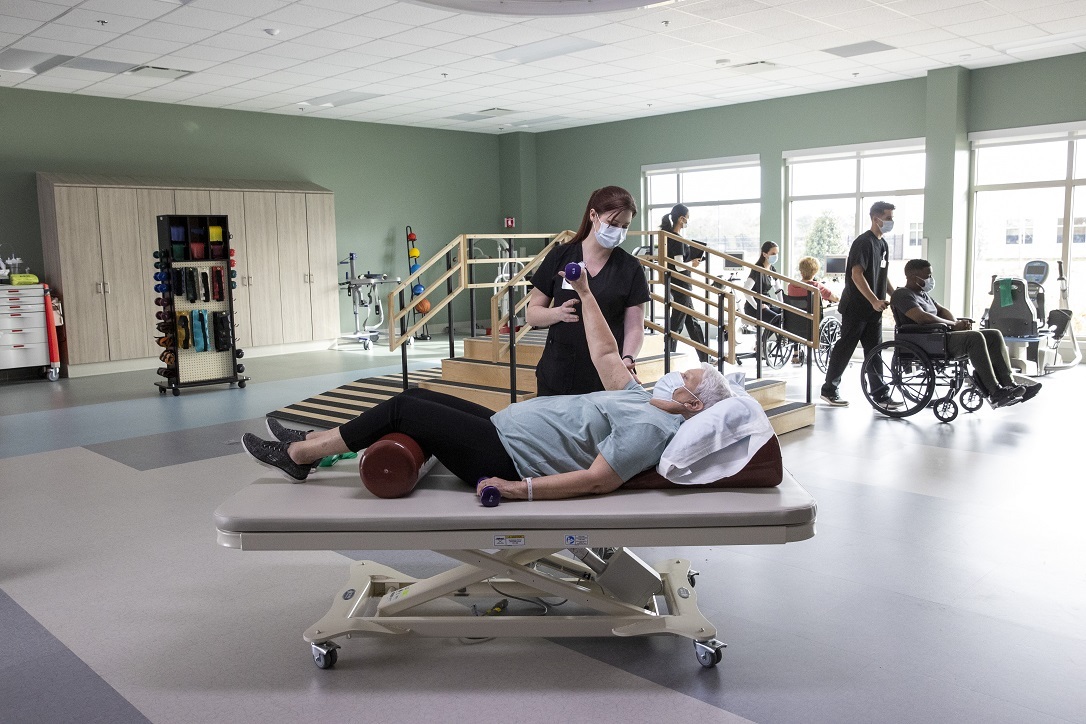
The Benefits of Exercise
Strength exercises and stretching are commonly prescribed by therapists in stroke recovery. Your exercise program might include:
- Aerobic exercise to improve endurance and walking capacity. It’s also a boost for your cardiovascular health.
- Resistance training with light weights to rebuild strength and restore muscle function. Improved muscle function makes activities of daily living easier and improves quality of life.
- Flexibility exercises and gentle stretching to soothe muscle tightness after stroke, enhance range of motion and prevent contractures caused by spasticity.
Eating Well Aids in Recovery
A healthy diet can play an important role in preventing a second stroke, reducing inflammation and simply feeling better overall. Plus, avoiding foods high in sugar and sodium and drinking plenty of water can improve pain symptoms such as headaches.
If you are overweight, your doctor may encourage you to lose weight. That may seem overwhelming if you’re experiencing pain and still recovering, but know that a little can go a long way. Losing as little as five to 10 pounds can improve your health, so every step in the right direction counts.
In inpatient rehabilitation, a dietitian is part of your care team. They will ensure you are receiving the nutrients you need to participate in therapy and recommend long-term dietary changes to maximize your recovery.
Manage Your Stress Levels
Stroke recovery—or recovery from any life-changing injury or illness—can take a toll on mental health. Experiencing pain in recovery may add to your stress level, so it’s important to find ways to relax and reduce stress. Exercise and a healthy diet helps, but there are other methods that can improve your mood.
Yoga is a good complement to physical therapy because it incorporates breathing exercises to help you relax, which can decrease pain. The postures can also promote flexibility and balance.
Consider incorporating meditation into your daily routine. Not only can meditation help reduce blood pressure, but there is also evidence that it can help manage insomnia, depression and anxiety. Even if you’ve never practiced meditation before, it’s easy to get started. Simply start by sitting quietly and focusing on your breath. When your mind wanders, gently bring it back to your breath again. Gradually increase the amount of time you’re able to stay focused.
Find Support
You don’t have to go it alone. Stroke survivors may feel better by speaking to others in similar situations. Support groups can provide information and a sense of belonging to help you reclaim your life and develop more independence. Ask your healthcare provider about support groups near you or use this tool from the American Stroke Association.
The Leaders in Stroke Rehabilitation
We are committed to delivering the highest quality care to help patients return to what matters most.
Learn about usThe content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.



