A hip fracture, or broken hip, can be a painful injury that takes time to recover from. As you age, the likelihood of having a hip fracture increases, especially for women and those with osteoporosis.
If you or your loved one does fall or have an accident that results in a broken hip, there are measures that can be taken to heal and regain movement and mobility after the injury.
What is a Hip Fracture?
Hip fractures are any break or crack in the upper thigh or general hip area, including the pelvis. Hip fractures are most common in older adults, and are often the result of a fall. According to the CDC, more than 300,000 adult seniors are hospitalized for a hip injury each year, with falls causing 95% of them.
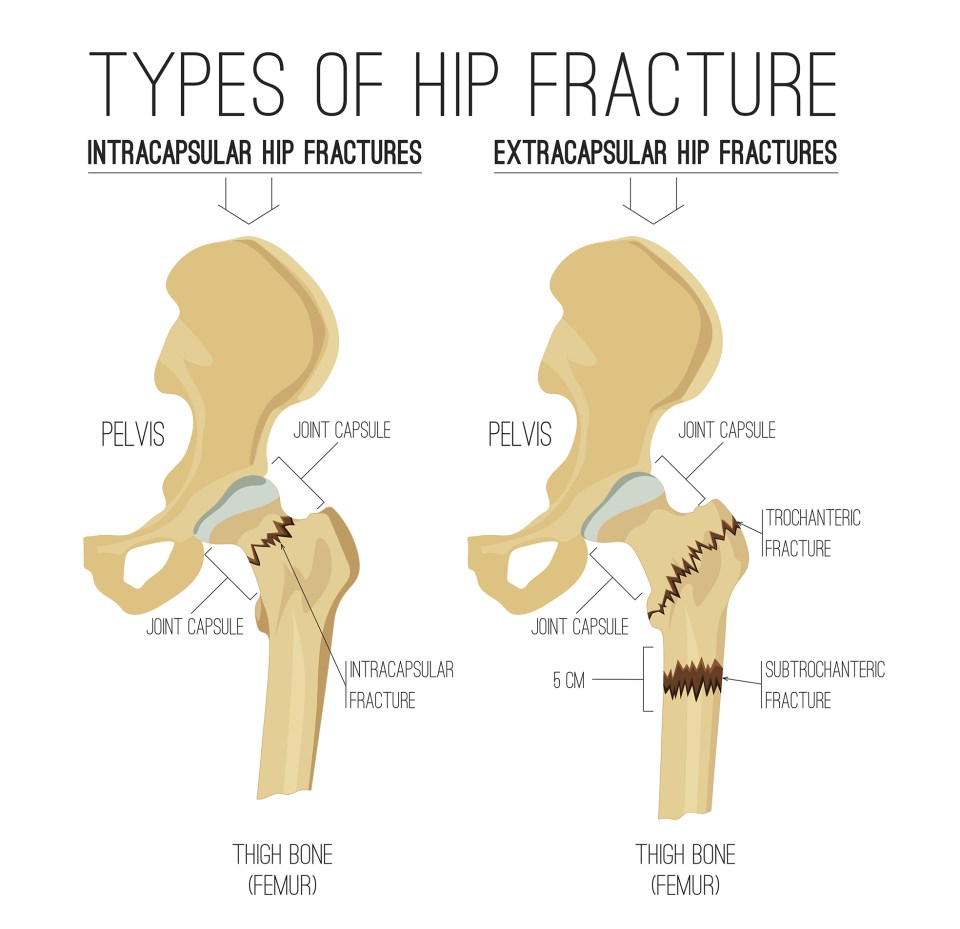
The two most common types of hip fracture are:
- Intracapsular hip fractures – a break or crack above the hip joint
- Extracapsular hip fractures – a break or crack below the hip joint
Can a Hip Fracture be Prevented?
With falls causing the majority of serious hip fractures, especially in older adults, Brandon Jackson, a physical therapist and head of the hip fracture program at Encompass Health Rehabilitation Hospital of Sewickley in Pennsylvania, said the best way to prevent a hip injury is to prevent a fall in the first place.
“There are basic things people can do in the home, like removing throw rugs and removing items on the floor,” he said. “You might want to have grab bars and other assistive devices installed in the restroom and house, as well.”
Watch out for some of these common fall risks in and around the home:
- Pets (large and small)
- Electrical cords
- Uneven floors
- Wet tile floors
- Area and throw rugs
- Improper footwear
- Steps and stairs
- Outside surfaces
- Unsafe/unsecured rails
- Visual distortions (low light, low contrast floors and steps)
- Clutter and obstacles (toys, etc.)
- Frequently used objects on high or low shelves
- Slippery tub or shower surfaces
While there are clear environmental fall risks in and around the home, other internal risks that increase the likelihood of a hip fracture are not as obvious. Many patients with hip fractures have other conditions, such as high blood pressure, arthritis and osteoporosis, that can either lead to a fall or make them a higher risk to suffer a broken hip as a result of a fall, Jackson said.
“Vitamin D deficiency, we’ve noticed, can also be correlated to fractures and weak bones,” he added. “Talk to your doctor and see if you need a supplementation.”
It’s also important to exercise regularly to prevent a fall later in life, Jackson said. “Exercise in general and staying as active as possible can help prevent a fracture in the future,” he said.
Hip Fracture Treatment
Hip fractures, especially in older adults, will likely require an acute hospital stay and possibly surgery. Surgical options include:
- Full hip replacement where the ball and socket of the hip are replaced with artificial parts
- Partial hip replacement where parts of the ball or socket are replaced with artificial parts
- Insertion of metal screws to hold the bones together while the fracture heals
After surgery, your doctor will likely recommend intensive therapy to help you heal properly and manage pain. Jackson said most of those recovering from a hip fracture can benefit from the services offered at a rehabilitation hospital.
What is a Rehabilitation Hospital?
Rehabilitation hospitals, such as Encompass Health, offer a hospital level of care combined with therapy to help patients recover their highest level of independence after an injury or illness.
Patients at a rehabilitation hospital receive three hours of therapy a day, five days a week from physical, occupational and speech therapists. Round-the-clock nursing care is available, and rehabilitation physicians visit frequently. The multi-disciplinary team will design an individualized care plan, setting specific goals, and ensuring each patient receives the right combination of physical, occupational and speech therapy.
How Hip Fractures are Treated in a Rehabilitation Hospital
The rehabilitation plan will depend on the patient’s weight bearing status – whether partial or whole weight bearing can be tolerated. The therapists will do an assessment upon admission to see how the patient moves.
Patients usually arrive at a rehabilitation hospital three to four days after surgery. They may still be groggy from anesthesia, so initial therapy is light, yet still meets the three-hours a day, five days a week requirement. Therapy will be spread out throughout the day, so patients can have needed breaks and rest. During the early part of the stay, Jackson said that pain management is a focus.
“In therapy, we talk about managing pain through repositioning and using heat and ice,” he said. “We also talk about the benefits of movement and mobility. That can help manage pain, as well.”
Therapists will work with patients on transitioning out of bed to a standing or sitting position, depending on whether they can bear weight. They’ll also work on using any adaptive equipment that might be needed, whether it’s a cane, walker or wheelchair.
Physical therapy will focus on activities and exercises that will be build strength, mobility and balance, while occupational therapy will focus on activities of daily living, such as dressing and basic hygiene.
If the patient can bear weight, Jackson said they want to get them up and moving around as much as possible. At Encompass Health Sewickley, he said they have a Walk with Me program, which gets patients up with the assistance of nursing staff even when they are not in therapy, Jackson said.
What Equipment/Technology is Used?

Jackson said they’ll work to build strength and mobility using a variety of equipment and technology.
An exercise bike, or enhanced equipment such as the MOTOMed or NuStep, can help build strength in both the legs and the core. The Bioness Integrated Therapy System uses a motion sensor to track patient movements as they perform certain exercises to build balance.
How Involved is Family During Rehabilitation?
Family members and loved ones are an essential part of the care plan. Depending on the hospital’s visitation policies, the primary caregiver may be invited for frequent meetings with the care team.
During that time, clinicians can teach caregivers about adaptive equipment that may be needed when their loved one returns home and provide them with any training that might be needed.
“We try to get them involved early on to provide them any education they might need,” Jackson said. “We want them to feel safe with their loved one at home too. We’ll give them recommendations, and we’ll also confirm the setup of the house. We want everyone to be ready at the time of discharge.”
The average length of stay for a hip fracture patient is typically around 10 to 12 days. After that, Jackson said that most patients able to be sent home with exercises to help them continue to heal. Depending on the severity of the fracture, the patient may also continue therapy with home health or outpatient therapy following their rehabilitation hospital stay.
What Should You Look for in a Rehabilitation Hospital?
Look for a hospital that has a specialized program for hip fracture recovery, Jackson advised.
The Joint Commission is the nation’s leading accreditation agency for healthcare and offers Disease-Specific Certifications. A TJC Disease-Specific certification indicates that the hospital’s program “meets the rigorous standards of the world’s preeminent accreditation and certification organization.”
“If you’re going to a place that has that seal, it means they have been vetted in terms of positive patient outcomes, and they’re continuing that process of improvement,” Jackson said. “The highest level of care and input is put into these programs. In my opinion, the whole point of getting the TJC Disease-Specific certification is to improve patient outcomes and experiences.”
For more information on hip fracture recovery, find an Encompass Health Hospital near you and talk to one of our rehabilitation specialists.
The content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.