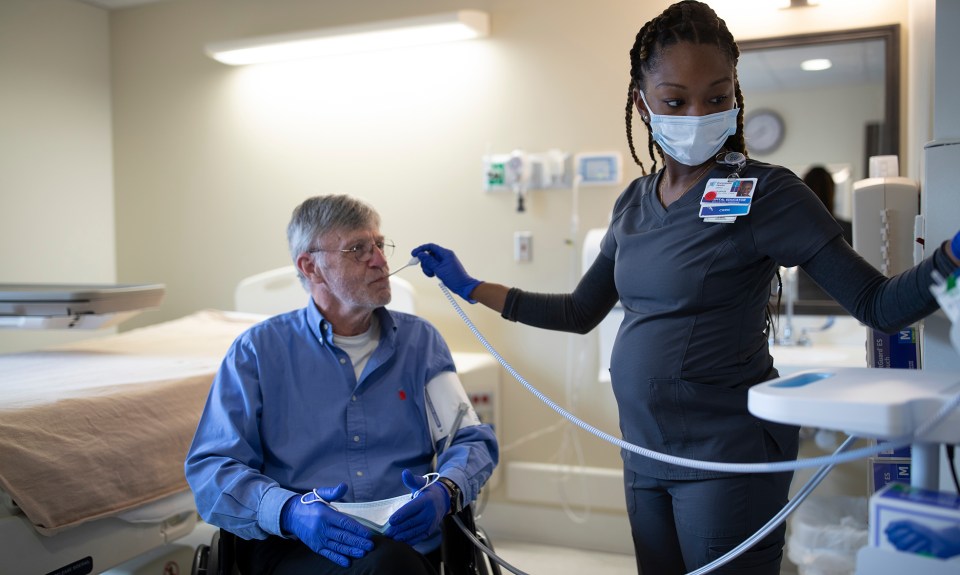
At this very moment, thousands of moms, dads, sons, daughters and cousins are able to be at home with their families because of rehabilitation.
Patients are admitted to rehabilitation hospitals to receive an intensive level of care from at least two disciplines of therapy (physical therapy, occupational therapy or speech language pathology) and require medical care from rehabilitation physicians, nurses and other disciplines. Case managers work to pull it all together to help move the patients along throughout their stays and to prepare for seamless discharges.
The first three words of this paragraph—patients are admitted—describe one of the most important roles that nurses play during the patients’ rehabilitation hospital stay: admitting patients. However, the role of nurses in rehabilitation doesn’t end there. Nurses play a critical role throughout the patient’s stay.
At Admission
RNs perform a thorough admission assessment covering all body systems, including history of illness and present condition. Not stopping at the physical assessment and history taking, rehabilitation nurses dig deeper into a patient’s cognitive and physical function to help determine the patient’s baseline in key performance indicators.
From the moment of arrival, observations of patients’ ability to perform the simplest tasks such as eating, bathing and dressing are in the works. Because nurses are the first clinician to evaluate the patient’s cognition and physical function, nurses set the initial plans of care related to patient safety in the first day of the stay. The rehabilitation nurse may determine that the patient’s inability to sit unsupported for five seconds combined with a high fall risk score indicates the need for safety interventions to prevent falls. Interventions would then be put into place immediately based on the plan of care generated by the nurse.
A Career You Can Trust
Encompass Health is committed to nursing growth and excellence in patient care. We stand apart with our exceptional work-life balance and great rewards. There’s never been a better time to join Encompass Health.
Learn MoreDuring the Stay
Throughout a patient’s stay, nurses conduct physical assessments every day, monitor the patient’s medical condition, administer medications, conduct education, and observe and document functional performance as indicated. Nurses work as part of the interdisciplinary team to adjust the plans and interventions to keep patients safe while helping them improve their physical function and cognition.
Rather than providing all of the care for the patient, rehabilitation nursing staff encourage patients to do as much as they can for themselves. This helps the patient practice skills learned in therapy and prepare to go home.
Preparing for Discharge
Nurses working around the clock provide a wealth of information and insight to the interdisciplinary team about how the patient can perform activities outside of the therapy gym. Patients may have more energy in the daytime to walk and transfer from the bed to the chair, but by nightfall, fatigue diminishes their endurance. Serving as a realistic preview of function in the home, these shared observations help guide the team in setting treatment plans and goals to facilitate the patient’s safe return home.
Why I Chose Rehabilitation
I found rehabilitation by accident—my own. I broke my ankle in several places and was unable to walk until receiving the expert care of a physical therapist. When I was at my lowest as a patient, unable to do anything for myself that required walking or standing, this physical therapist came along and brought me out of my doldrums.
The physical therapist’s ability to help me learn to help myself was such a revelation. What was this practice of rehabilitation? One thing led to another and I became a rehabilitation nurse.
After 27 years as a rehabilitation nurse I am still amazed at what we do: helping people learn to help themselves and their loved ones. Sometimes all we need is to be informed and pointed in the right direction. I am glad someone pointed me in the direction of rehabilitation nursing.
The content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.