*This article was originally published by ASHA’s Leader Live, and is written by Encompass Health Rehabilitation Hospital of Vineland’s Allison Frederick
I like to think of myself as a prepared person. I’m not a fan of the unknown, so I like to know what to expect and have a plan. It eases my anxiety. So when the COVID-19 pandemic began to take over the state, I prepared by doing all the reading and research I could. But nothing could have prepared me for when the virus invaded southern New Jersey.
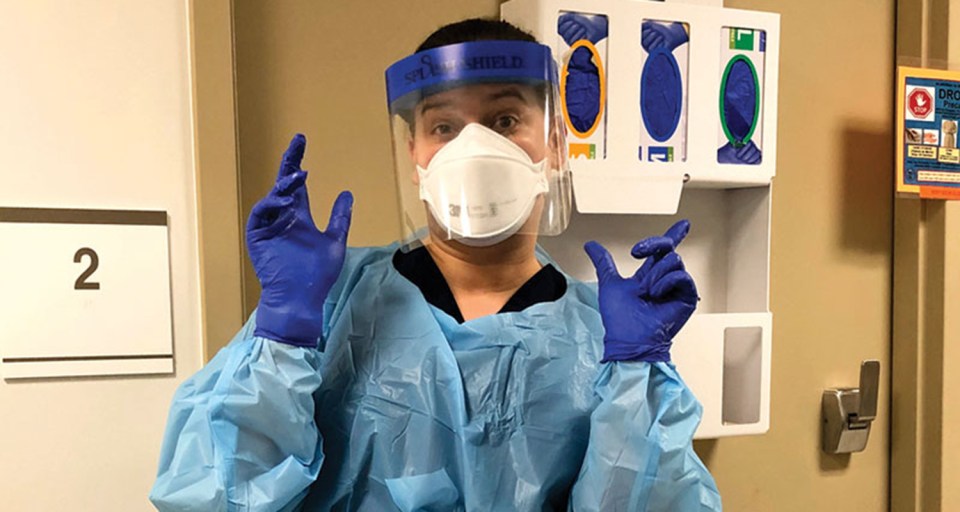
I work in acute rehabilitation, so we were getting patients who were recovering from COVID-19 as a primary diagnosis, and also those who had acquired it while hospitalized for something else. I volunteered to be the speech-language pathologist for our COVID-19 patients. I live alone, so I didn’t mind being the designee. Learning the new personal protective equipment procedures was daunting and overwhelming, but I quickly got into a decent routine.
The first day I treated one COVID patient, and thought, “OK, that wasn’t so bad. This is manageable.” Then it snowballed—from one, to two, to seven—and things started to get … complicated. And I’m not just talking about caseload management. I’m talking about my own mental health.
Everyone at work was on high alert, and people were morphing into scary versions of themselves, with short fuses and negative attitudes. New Jersey was essentially on lockdown, and I couldn’t go anywhere except work or my house, meaning the only people I saw were my equally anxious co-workers. I had no reprieve from the chaos that was work.
I felt extreme guilt continuously, because my situation wasn’t as bad as that of other speech language pathologists: guilt that I was working in rehabilitation instead of a hospital, which meant I didn’t see people dying. Guilt that co-workers were furloughed.
At home, I was alone all the time. I don’t care what anyone says—FaceTime and Zoom do not replace human interaction. I wasn’t sleeping, and felt a deep, aching sense of dread every morning.
A friend finally had what I like to call a “come to Jesus” talk with me about my current mental state. I needed therapy. I already take antidepressant medication, but it wasn’t cutting it. I decided to visit a therapist.
I wasn’t crazy about the idea of teletherapy, but I quickly warmed to it. The therapist gave me the tools to manage my anxiety in real time and gave me a new perspective: I am not responsible for other people’s feelings. I don’t need to protect everyone. I just need to protect myself and manage my own feelings. Therapy did that for me.
I take comfort in knowing that if (or more likely when) the second wave comes, I’ll be better prepared to care for myself because of my experience with teletherapy. I can’t help anyone else if I’m not taking care of myself, and I need to keep that in mind to best serve my patients and co-workers.
Allison Frederick, MS, CCC-SLP, has been working in acute rehabilitation for 10 years, with a focus on acquired brain injury. She is also a regular contributor to the ARC Seminars inpatient rehabilitation blog. allison@arcseminars.net
The content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.