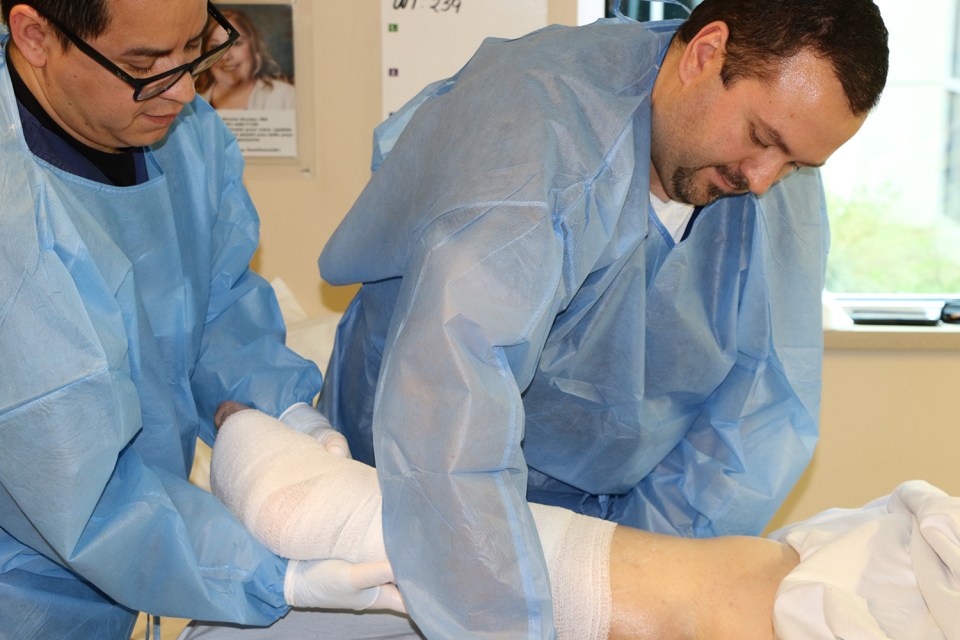
When people think of wound care, they often think of a traumatic injury where treatment is provided to control bleeding and decrease risk of infection. Wound care treatment in the inpatient rehabilitation setting is actually quite different than emergency care and has a stronger focus on prevention and education.
At Encompass Health Rehabilitation Hospital of Toms River, patients who require wound treatment are usually admitted to our hospital with existing wounds and have received some sort of initial treatment in the previous setting. Once here, our goal is to facilitate healing, promote nutrition, provide education on prevention and treatment and prepare for discharge home.
The most common wounds we see are pressure injuries and traumatic wounds. We also regularly see burns, moisture related skin damage, diabetic wounds and wounds from arterial or venous disease.
We decided to establish an interdisciplinary wound care team at Encompass Health Toms River in 2015, as our patient population became more complicated and their wounds become more frequent and complex. In 2017, our wound care program received Disease-Specific Certification by The Joint Commission and was recently recertified in June.
So what exactly does a wound care program look like in inpatient rehabilitation? The following is a quick look at what wound care is and isn’t in inpatient rehabilitation.
Common misconceptions about wound care
- I put on Band-Aids all day. Although half of my job does revolve around physical treatment and application of dressings, the other half focuses on prevention. Some of the most important work we do as wound care coordinators involves educating the staff and patients to prevent wounds from happening.
- It’s the nurse’s job. Wound care involves the whole interdisciplinary team. In our hospital, every department is integral in treatment and prevention. For example, our respiratory therapists perform a skin inspection on admission for any patients with respiratory devices. A successful wound care team involves everyone. It is a collaborative effort. Our team has members from the medical staff, nursing, physical therapy, occupational therapy, infection control, quality and risk management, dietary, case management and respiratory therapy. Wounds are not just topical care. Your skin is your biggest organ system and requires a lot of attention. Repositioning, treatment, support surfaces and nutrition are critical to wound care and a safe discharge home.
What role does prevention/education play in wound care?
Prevention and education may be just as important as the actual treatment. You can put the most expensive dressing on a wound, but if you do not treat the cause, the wound will not heal. Patients have to understand why the wound happened. Prevention of pressure injuries is critical. Each patient is assessed on admission and receives a risk score for developing pressure injuries. High risk patients (even those without wounds) are being followed by the wound care team to assure they are receiving appropriate nutrition supplementation and pressure redistribution devices (ex. wheelchair cushion, low air loss mattress, heel suspension devices).
What’s the importance in having TJC certification for your wound program?
A certification from The Joint Commission means an outside credentialing body has assessed your program and given a gold seal of approval. They look to see that programs are practicing based on established clinical practice guidelines. It assures patients they are receiving treatment based on evidence-based practice. They also require programs to choose areas of improvement, collect data and monitor trends.
The content of this site is for informational purposes only and should not be taken as professional medical advice. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding any medical conditions or treatments.